New report determines in-home patient care can save an average of 22% over inpatient care for six different health conditions
Momentum continues to build in favor of the “Hospital in the Home”, known by the acronym HITH. For certain health conditions, this care model allows the patient to remain in his or her home, instead of staying in a hospital. Caregivers, including specialist physicians, come to the residence with almost the same frequency as occurs for hospital inpatients.
Wider adoption of this model of patient care would directly affect pathologists and clinical laboratory managers who work in hospital laboratories. Over time, it could mean fewer inpatient admissions and thus, less medical laboratory test volumes for inpatient services. On the other hand, more HITH patients would increase the need to collect specimens in patient’s homes and get them to a local clinical laboratory for testing. Hospital-based medical laboratories—because they are central to the communities they serve—would be well-positioned to provide this diagnostic testing.
Cost savings are substantial, and patient outcomes are consistently as good, if not better, than the outcomes of hospital inpatients who are treated for the same conditions. In Australia, a new study of hospital-in-the-home services affirms these benefits. Researchers determined, that for six specific health conditions, HITH care would cost an average of 22% less than hospital care. That is a substantial savings per patient and shows how the HITH care model could help control the increasing cost of healthcare.
The study was commissioned by the Hospital in the Home Society of Australasia, Ltd. and was conducted by Deloitte Access Economics. The authors of the report, titled “Economic Analysis of Hospital in the Home”, argue that patients prefer being cared for at home rather than in hospitals. In Australia, advocates for hospital in the home (HITH) programs are using this report to lobby for an extensive expansion of services that provide hospital-type care in private residences. Patients treated in HITH often have:
- a common condition (e.g., genitourinary, respiratory, skin, joint and soft tissue infections, and thrombo-embolic disorders);
- a relatively uncomplicated diagnosis; and,
- well-defined treatment that is safe to deliver at home.
The range of conditions treated using the hospital-in-the-home care delivery model include the following:
- treatment of infectious diseases (e.g., endocarditis, septic arthritis, pneumonia, treatment of cellulitis using intravenous antibiotics);
- treatment of diabetes and diabetic complications, respiratory failure, and complex chronic illnesses;
- provision of parental nutrition, blood transfusion, and percutaneous endoscopic gastrostomy where services are usually provided in acute inpatient settings;
- complex wound care and ulcer management;
- the provision of cardiac treatment and rehabilitation (e.g., the post-operative management of patients after cardiac surgery, atrial fibrillation, endocarditis);
- home infusion therapy including chemotherapeutic agents, antibiotics, analgesics, immunologic agents and enzyme replacement;
- oncology and palliative care; and
- post-surgical care (e.g., knee replacement, repair of fractured hips, breast surgery).
Many of these health conditions require clinical laboratory testing at regular intervals to monitor patient progress. At the same time, the need to send phlebotomists and similar health professionals to patients’ homes to collect specimens would create new operational challenges for hospital-based laboratories that wanted to support the HITH care model.
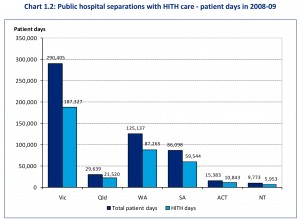
This bar chart, presented in “Economic Analysis of Hospital in the Home,” shows, by Australian state, the number of patient days of care provided in the form of hospital-in-the-Home services during 200809-09. The State of Victoria is the largest user of the HITH care model. During this period, it had 290,405 patient days of HITH care
“Patients are visited every day by nursing staff and two or three times a week by specialists,” observed Gideon Caplan, M.D., who is President of the HITH Society. “[This is] the same as they would if they were in a traditional hospital setting. We believe you could double the number of patients using the services and, in coming years, tens of thousands of extra patients could be suitable.”
Caplan has been providing home care for Sydney’s Prince of Wales Hospital since 1995. He is also an Associate Professor at the School of Public Health and Community Medicine at University of New South Wales in Sydney.
Rising HealthcCare Costs Spur Interest in Promoting In Home Treatment
Among the benefits of hospital in the home care gleaned from the Deloitte analysis are:
- caring for suitable patients in their own homes cuts costs by nearly one-third;
- delivering the same health outcomes as the hospital;
- freeing up beds in hospitals for the patients who need them most;
- enabling hospitals to focus on doing more elective surgery;
- reducing patient risk for infection; and
- taking pressure off hospital emergency departments.
According to Caplan, disincentives to doctors participating in the service should be removed from the country’s health care system, including restrictions on general practitioners claiming healthcare payments for patients who were classed as hospital patients. “If I’m working in a hospital and do rounds, I can see patients. Obviously, you can’t do that if you’re visiting people in their homes,”’ he said. “Specialists get paid more for seeing patients in hospital than at home but really it should be done the other way around.”
Most of the states and territories in Australia, in response to rising healthcare costs already provide acute, sub-acute, and post-acute care in the home. The Deloitte report noted that this in-home care is made possible by portable technology. It found that hospital in the home care was cheaper for several health problems listed on country’s admitted patient classification system (Australian Refined Diagnosis Related Groups or AR-DRGs). This system provides a clinically meaningful way of relating the number and type of patients treated in a hospital to the resources required by the hospital.
The six specific health issues examined in the Deloitte report were cellulitis, venous thrombosis, pulmonary embolus, respiratory infection, inflammation, chronic obstructive pulmonary disease (COPD), and knee replacement. Caplan noted that, making the switch to hospital separations for those patient conditions would save the government $108.6 million, even with nursing staff and specialists visiting patients at home two or three times a week, similar to the traditional hospital.
HITH care was found to be less costly than hospital care for all AR-DRGs except COPD, where it was estimated to be 6% more expensive; and the greatest potential cost savings were associated with expanding HITH care for cellulitis. The Deloitte study demonstrated the importance of adjusting for factors that can influence the cost-effectiveness of HITH; and it concluded that the relative costs of HITH depends on context and diagnosis.
Pathology Laboratory Service Will Not Be Spared as Hospital in the Home Expands
One significant finding among the health care cost savings is that HITH care may reduce pathology service use; but, according to an Australian and New Zealand Journal of Public Health article by Caplan and others more than 10 years ago, it is difficult to quantify the hospital resource savings that would result. The pathology cost center, Deloitte includes in its report, illustrates the cost of salaries or wages of those administering tests and the cost of test supplies. While fewer pathology tests will reduce consumption of test supplies, it is unclear whether it would result in salary cost savings. This report assumed that the same pathology costs would apply to a HITH care separation and a hospital care separation.
Deloitte Access Economics’ study of several other reports found no significant differences between mortality outcomes for hospital in the home patients and those who stayed in a hospital ward. Critics of the HITH model argue that the approach is simply an invitation for inferior care; however, hospital in the home is a response to consumer preferences, even though studies found that hospital readmission rates for older HITH patients with a mix of medical conditions did increase.
—Carren Bersch
Related Information:
Economic Analysis of Hospital in the Home—report by Deloite Access Economics
Hospital house calls could cut expenses
Hospital house calls cut spending by a third, reports says


